NORTHERN NEVADA’S
PREMIER EYE DOCTORS
Leaders in experienced, state-of-the-art medical and surgical care for the eyes.
CONDITIONS TREATED
Comprehensive Solutions for Low Vision in Reno, NV
What Is Presbyopia?
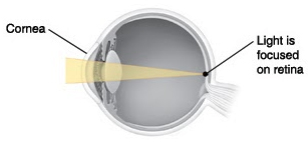
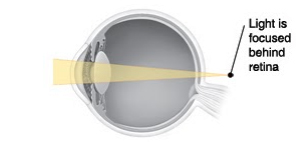
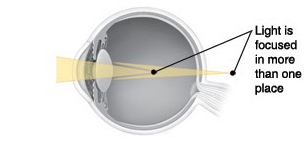
Presbyopia is the loss of close-up focusing. Normally, the lens in the eye changes shape to focus light directly on the retina (back of the eye). But with age, the lens hardens and cannot change its shape as easily. It then can’t focus clearly on close objects. This makes them look blurry.
Presbyopia makes it hard to do things close up, such as read small print, use tools, or thread a needle. The first sign may be a tired feeling when you look at something close up. Medical eye care can help you manage presbyopia and recommend corrective options. Presbyopia most often starts when you’re 40 to 45 years old. It slowly gets worse until you’re about 60 to 65.
What Is Low Vision?
When you have low vision, you need more than glasses or contact lenses to see well enough to get around and do day-to-day tasks. Your central or side vision, or both, may be reduced.
What Causes Low Vision?
Low vision can be caused by a number of diseases in the eye. An injury to the eye can also result in low vision. And some people are born with low vision. If you’re dealing with low vision in Reno, NV, we offer solutions tailored to help improve your quality of life.
What Are the Symptoms?
The symptoms of low vision depend on the cause of the vision loss and where the problem is in the eye. Symptoms can include:
- Blank spots, dark spots, or wavy lines in the center of your vision
- Blurred, hazy, or cloudy vision or double vision
- Loss of side (peripheral) vision or color vision
Eye Movements with Nystagmus
With nystagmus, eye movements are quick and repetitive. They can be continuous (all the time) or paroxysmal (happening “on and off”). They are always involuntary (not controlled by the person). The direction of eye movements can be:
- Horizontal (side to side)
- Vertical (up and down)
- Rotary (around in a circle)
- See-saw (one eye goes up while the other goes down)
- Any combination of the above
Because of these abnormal movements, the eyes can’t focus well. This impairs vision. To see better, a person may hold the head in an unusual position. This is done to access the “null point.” This is an angle of vision that helps limit abnormal movement of the eyes. A person may also nod the head to reduce eye movement. Medical eye care can help manage these symptoms and provide treatments to improve vision.
Types and Causes of Nystagmus
There are two main types of nystagmus. Each type can have one or more causes. But the exact cause is often unknown. Most cases of nystagmus are permanent.
- Congenital (or infantile) nystagmus. This is the most common type. The child is born with it. Symptoms appear soon after birth. This type has two main causes: sensory problems and neurologic problems. It can also be linked to other health conditions.
- Sensory problems. Vision problems such as cataracts (a clouded lens of the eye) or glaucoma (increased pressure within the eye) may be a cause of nystagmus. Another possible cause is a problem with the retina (the light-sensing layer of nerves that lines the back of the eye) or the optic nerve (the nerve that connects the eye to the brain).
- Neurologic problems. Problems in the brain can cause nystagmus. This is because the brain and the eyes must work closely together to make good vision possible.
- Other conditions. Albinism (lack of pigment in the skin and eyes) and aniridia (absence of the iris of the eye) are linked to nystagmus.
- Acquired nystagmus. This type is not present at birth. It has several possible causes. These include:
- Alcohol use
- Use of certain medications (most often anti-seizure medications)
- Inner ear disorders, such as Meniere’s disease
- Disease in the brain, such as multiple sclerosis or a brain tumor
- Stroke
- Injury to the head
Symptoms of Nystagmus
Symptoms depend on the type of nystagmus. With the congenital type, impaired vision may occur. But the eye movement may not be bothersome. With the acquired type, the eye movement may be more pronounced and bothersome. Blurry vision may occur. Also, depth perception may be affected. This can impair balance and coordination. It can also cause dizziness.
Diagnosis of Nystagmus
The doctor or eye care provider will take a health history. A physical exam, including an eye exam, will be done. And certain tests may be done. These include:
- CT (computed tomography) or MRI (magnetic resonance imaging) scan of the head. These imaging tests create pictures of the brain. They can show any swelling, stroke, or tumors that may be causing nystagmus.
- Electro-oculography (EOG). This tests the function of the retina. It does this by recording movement of the eyes.
- Vestibular testing. This checks for problems in part of your inner ear (the vestibule). This part of the ear helps control eye movement.
- Lab tests. These check for infections, an imbalance of chemicals in the body, and tumors.
Treatment of Nystagmus
In most cases, treatment helps reduce symptoms but does not eliminate them. Treatment depends on the cause of the nystagmus. There are five main treatment options:
- Treatment of the underlying cause. If there seems to be a clear cause, it is addressed. For instance, a cataract is treated or a tumor may be removed. If a medication is the cause, it may be stopped or replaced. Unlike with other causes, when these underlying causes are treated, nystagmus may be cured.
- Treatment of related vision problems. For instance, contact lenses or eyeglasses can help correct problems such as near- or farsightedness. Special prisms may be used to adjust the gaze. This helps reduce symptoms.
- Medications. These can help reduce symptoms, such as eye movement and vision loss.
- Botulinum injections. These weaken certain muscles within the eye. This helps reduce symptoms.
- Surgery. This procedure alters the position of the muscles that move the eyes. It does not cure nystagmus, but may reduce the amount the head needs to turn to see best.
Understanding Ocular Histoplasmosis Syndrome (OHS)
Scientists believe that OHS is caused by Histoplasma capsulatum (H. capsulatum). This fungus is found in the dust and soil in parts of the U.S. (mostly the Mississippi-Ohio River Valley area). If breathed into the lungs, the fungus can cause histoplasmosis. This is typically a mild condition with flu-like symptoms or no symptoms at all. The condition often goes away without treatment. But it is thought that once in the body, H. capsulatum can also affect the eyes. This is OHS.
OHS causes inflammation in the choroid. This is the layer of blood vessels in the retina (the light-sensing layer of tissue at the back of the eye). The inflammation leaves scars called “histo spots.” As OHS progresses, abnormal blood vessels can grow at the histo spots. These blood vessels form lesions called choroidal neovascularization (CNV). If the CNV lesions leak blood and fluid into the macula (the center part of the retina that plays a key role in clear vision), vision can be distorted. More seriously, if the lesions occur in the macula, vision loss can result. If OHS occurs in one eye, it may later occur in the other eye.
Risk Factors for OHS
Anyone who has had histoplasmosis is at risk of OHS. But very few people develop OHS.
Signs and Symptoms of OHS
Early cases often have no symptoms. But as the disease progresses, an eye doctor may find histo spots during an eye exam. And a patient may notice vision changes such as:
- A blind spot in the eye
- Straight lines appearing crooked or wavy
Diagnosis of OHS
An eye doctor can check for OHS. Your pupils (the dark circles in the centers of your eyes) will be dilated (enlarged) with special drops. Your eyes will then be examined. Fluorescein angiography may also be done. With this test, a special dye (fluorescein) is injected into a vein in your arm. The dye travels to your retina. The dye allows the doctor to check blood flow to the retina. This helps the doctor see any histo spots.
Treatment of OHS
If the macula is not affected, OHS does not need treatment. When the macula is affected, there are two types of treatment:
- Photocoagulation. With this surgery, a special laser destroys the abnormal blood vessels in the retina. This procedure can only help protect against future loss of vision. It cannot repair vision loss that has already occurred.
- Medications. These limit abnormal blood vessel growth. The eye is numbed and then injected with medications. These injections need to be repeated every 4 to 12 weeks. The frequency depends on the type of medication used. Your doctor can tell you more about this treatment.
Checking for Macular Damage
Your eye doctor may suggest that you use an Amsler grid. This can be helpful for patients who have already had laser surgery, as well as those with histo spots but no vision loss. An Amsler grid is a simple lined grid with a dot in the middle. Looking at it can help you check for signs of damage to the macula. If damage has occurred, the lines of the grid may look curved, or a blank spot may seem to appear. Our specialist can guide you through using the Amsler grid and help detect macular damage in Reno, NV.
If you’re experiencing any vision concerns or need expert advice, don’t wait. Contact us today to schedule an appointment with our experienced eye care professionals in Reno. We’re here to provide personalized care and solutions for all your eye health needs.